BY BRADLEY NORTHCOTE

(Courtesy Speakers’ Spotlight)
Stéphane Grenier retired from the army, but there’s a battle he will continue to fight.
The retired 29-year veteran of the Canadian military, who has served in several countries, most notably including Rwanda and Afghanistan. delivered a message to the Sheridan community Monday night at the Davis campus in Brampton: a clinical approach to mental health is not enough.
While he started out promoting peer support among members of the Canadian military, Grenier says the problem is much broader.
He sees his military service as significant for his own mental health experience.
“For me, it was the beginning of the rest of my life,” he said of his service in Rwanda under another Canadian serviceman, Lt. Gen. Roméo Dallaire, who wrote the best-seller Shake Hands With the Devil about his own experiences in Rwanda and his struggle with Post-Traumatic Stress Disorder (PTSD).
Grenier’s now ex-wife said at the time of his return from Rwanda that he “had a mistress, and her name was Rwanda,” a remark he found painfully true.
For Grenier, it’s not PTSD, but depression that is his greatest struggle. He’s not an outlier. Statistics Canada’s 2013 Canadian Forces Mental Health Survey showed symptoms of depression were the most commonly reported mental health struggle throughout the prior year, although rates for PTSD doubled since 2002 while those for depression remained about the same.
Since returning to Canada, he has put his experience in perspective by investigating the mental health support available to average, non-military Canadians. On a mission to help Canadians from all walks of life fight their own, sometimes silent, inner battles, he started Mental Health Innovations Consulting (MHIC) in 2012.

MHIC seeks to address what Grenier saw as a need to supplement clinical mental health care with strong peer support networks in workplaces and communities.
“I’ve moved on. . .You don’t have to go to war to have a mental health problem.”
You shouldn’t have to go to war to get proper support for mental health struggles, either, he told the crowd of 70 at The Den. He is candid about the gap left by clinical support, which he said can best be filled through peer support from family, co-workers, or others.
“My suicide attempts were not in my doctor’s office,” said Grenier.
He describes, to a hushed crowd, thoughts of intentionally crashing his car, and burning a suicide note after what almost became one attempt. This, he says, highlights how hiding our mental health struggles can add to the problem in a way medical doctors, unaware of unexpressed thoughts, can’t resolve.
“I’m not against doctors,” Grenier stresses. He does take medication, and won’t discourage others from doing so. The point, he said, is clinical help should be a supplement to, not a substitute for, support from peers.
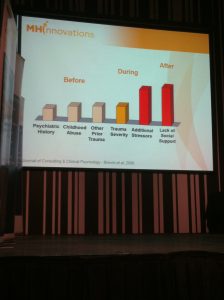
“The highest predictor of who will develop mental health problems is a lack of social support,” said Grenier.
He spent years going to work at a base in Valcartier, Quebec, crying but trying to keep it to himself. He went about his fatherly routine playing catch with his young kids, who he said could tell something was wrong. Later, a co-worker saw Grenier struggling and, though not asked, offered to guide him to help. As Grenier said, he “bumped into peer support.”
In 2000, six years after starting his mission in Rwanda, Grenier was diagnosed with PTSD and depression.
The peer support rather than the diagnosis, said Grenier, was the turning point. He said peer support along with clinical help through tough times is what matters.
He describes mental health as a continuum. This comes from his own experience, he says, as his suicidal thoughts didn’t appear suddenly.
Since mental illness doesn’t reach a peak crisis point overnight, and since silence can be a barrier to help before that point, he says, the solution can’t be found by waiting for a clinical label. Anyone could fall short of a clinical diagnosis but still be in need of help, facing a mental health struggle as he did for a time after his father died of cancer, he said.
“A mental health problem is not always a diagnosis. . .You have to stop seeing [bad days] through the eyes of the clinical system.”
How many times, Grenier asked the crowd, had they been asked “How are you?” and answered honestly? There were murmurs of agreement when he said we should go beyond saying “fine” and answer tactfully but honestly. The peer support resulting from an honest answer, Grenier says, could make a difference.
There’s one type of non-clinical support that Grenier regards with a healthy skepticism. Corporate awareness campaigns, he says, can be great for companies seeking free advertising, while not going far enough to offer concrete support. His response to Bell Let’s Talk: “We’ve talked enough. . .We can do more.”
This message is meant for Sheridan, too. While Grenier said he likes the concept of a friendship bench at Sheridan, he says he’s unsure if the bench always serves its intended purpose of starting discussions.
“I’m challenging your institution to do something tangible,” he said.
Grenier said he was thankful for tangible support that went into his talk at Sheridan. His appearance was one of six annual talks in the Creative Campus Series, which were “created to celebrate Sheridan’s commitment to creativity and innovation across disciplines.”
Looking Ahead
This year’s series is sponsored by TD Bank.
Sheridan’s Faculty of Continuing and Professional Studies (FCAPS) will carry out some initiatives of its own. It will continue the Creative Campus Series with a series of workshops held in collaboration with the Centre for Addiction and Mental Health (CAMH) at Studio 89 in Mississauga today. Working with staff from other organizations serving clients with health and social challenges, FCAPS will also be offering courses, from later this month until the end of April, on promoting good mental health in the workplace.
